2011-12-28
Janda first notes
Tags: Janda, Neurology, Functional
Role of muscles in musculoskeletal syndromes
Vladimir Janda MD , Dr SC
Functional pathology of the motor system is a term used to describe, in various musculoskeletal syndromes, the pathogenitical importance of the impaired function rather than the structural lesions. An impaired function is often associated with pain, both acute as well as chronic. However, the development may be latent for a long period of time (even years). On the other hand, pain always causes an impaired function. This concept helps to bridge the discrepancy in correlation between symptoms and structural lesions.
To understand the musculoskeletal syndromes, from the functional point of view, three stages of understanding can be differentiated:
- Joints and their dysfunction as a cause of pain,
- Muscles and muscle-joint correlations as a main cause of the syndrome
- Central nervous motor regulation, changes of movement patterns and quality of motor behaviour as a cause of (in particular) chronic pain.
Evaluation of the musculoskeletal system can be divided into two parts:
- The actual diagnosis or estimation of a direct pathology/dysfunction which caused the acute pain syndrome. Treatment has often a character of the first aid.
- Analysis of factors which may be considered as a presumption for acute decompensation. This analysis is important in particular from the point of view of prevention of recurrences of acute pain episodes or development of chronic pain.
In principle, three types of “pathology” of the motor system can be recognised:
- Structural
- Functional (hysterical)
- Organic, however expressed by impaired function of any part of the motor system. Morphological changes in such a case are negligible or almost negligible and certainly irrelevant.
In motor disturbances, two types of functional impairment are to be considered:
- Associated with a structural neurological lesion (alienation of Kenny in acute poliomyelitis, dormant motoneurons of Kabat in upper motor neuron lesions, such as in hemiplegia)
- Occurring in morphologically intact nervous part of the system, as it occurs in various musculoskeletal disorders. Most pain syndromes belong to this category and may constitute a special clinical entity. This category includes some injuries, such as unstable ankle joint after a sprain (foot way, Freeman).
Motor system functions as one entity. One of the basic presumptions of our concept is that the motor system functions always as one entity. Any lesion located anywhere is immediately reflected by adaptative responses in the whole motor system. Therefore, a strictly localised lesion of dysfunction does not exist. One of the presumptions of a successful rehabilitation is to slow down the fixation of these adaptive reactions and fixation of impaired movement patterns and pain patterns. The process of development of adaptive responses occurs at all levels of the motor system and is called centralization. These adaptive responses may even prevail and be the source of further decompensation, creating a vicious circle. This is a frequent situation in chronic pain syndromes, in which the original cause of pain can be recognised only with greatest difficulties, if at all.
There are four levels of the motor system at which the adaptive reactions seem to be the most evident:
- Cortical/subcortical regulatory centres,
- Segmental spinal cord regulation,
- Muscles
- Joints and adjacent structures.
Regardless at which level the problem starts, the final result is a generalised dysfunction and we speak about the rule of vertical and horizontal generalization.
The muscular level represents perhaps the most exposed and labile part of the motor system. As the main effectors, they must respond quickly to all changes or stimuli coming from the neural structures as well as to changes in the peripheral part, i.e. from the osteoacticular systems and skin and of course from the viscera.
Muscles should not be considered as a homogenous “flash” because all striated muscles are composed from fast and slow twitch fibres. It has to be accepted that in man, different muscles behave in different ways. Although it does not seem to be a histological correlation, clinically two types have to be differentiated: those prone to develop tightness and those prone to develop inhibition and weakness. The changed relationship between these two systems results in a muscle imbalance with typical clinical consequences. Muscles imbalance is therefore considered as a systemic reaction of the muscle system.
The most important signs of impaired muscle function which should be considered in relation to the musculoskeletal disorders are: the increased muscle tone (muscle spasm), muscle imbalance, muscle patterns associated with the joint dysfunction, motor units firing pattern associated with the muscle contraction speed as an important factor to prevent injuries of the joint system.
Increased muscle tone is considered as an important factor in the genesis of pain in the locomotor system. It is believed that a joint dysfunction results into a painful condition only in presence of increased tone in a muscle which is related (anatomically or functionally) to that particular joint. Terminology, pathophysiology and treatment of muscle hypertonicity are vague. From the clinical point of view, however, at least five types of increased muscle tone would be differentiated and this should be taken into consideration in treatment. These different types are: limbic, segmental (spinal cord), uncoordinated contraction resulting in trigger points, pain irritation and muscle tightness, which is associated with altered elasticity and changes of the connective tissue and results into muscle imbalance.
Muscle imbalance is a systemic change of quality of muscle which results into altered biomechanics and is associated with a gradual alteration of movement patterns. Muscle imbalance has to be considered as one of the important factors which perpetuate recurrences and chronic pain syndromes. In short, muscle imbalance can be described as an altered relationship and balance between muscles which are prone to tightness or inhibition.
Muscles with tendency to develop into tightness are: triceps surae, hamstrings, short thigh adductors, hip flexors (iliopsoas, rectus femoris, TFL), piriformis, quadratus lumborum, spinal erectors, pectorals, upper trapezius, levator scapulae, STM, short deep neck extensors.
Muscles with tendency to inhibition: tibialis anterior, vastus medialis, abdominal rectis, lower stabilisers of the scapula (serratus anterior, rhomboids, middle and lower trapezius, deep neck flexors (scalenes)).
The main consequences of imbalance between the two systems are: uneven distribution of pressures on weight-bearing joints as a presumption for dysfunction, pain and later on probably degeneration, decreased ROM and compensatory hypermobility, altered proprioceptive information followed by adaptive regulatory central nervous regulation (reprogramming).
Although muscle imbalance after all involves the whole muscle system, it usually does not involve all muscles to the same extent at the same time but develops gradually. There are two predilection areas where the imbalance starts to develop: the pelvic region resulting into a “pelvis (distal) crossed syndrome” and the shoulder neck region, resulting into a “proximal crossed syndrome”. The pelvic crossed syndrome results into overstress of the L/S junction. The proximal crossed syndrome results into typical changes of posture with overstress of the cervicocranial junction, the C45 and T4. Due to the altered axis of the glenohumeral fossa to the overstress of the shoulder joint.
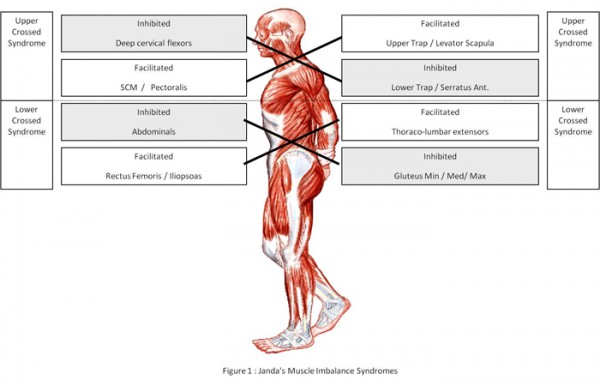
In addition to these two syndromes there is the later (stratification) syndrome which in principle is a combination of both crossed syndromes. It is a sign of an altered shape of the muscular system due to a long lasting dysfunction and is a sign of a bad prognosis.
Movement patterns and their evaluation is more important than estimation of muscle strength of individual muscles. The importance of inhibited and weakened muscles is not in their individual strength but rather that their activation is less and delayed.
In evaluation of movement patterns, the main concern is paid to timing (sequencing) of firing of muscles and degree of their activity. Muscles which are activated during a particular movement should be considered as synergists for the particular movement as they get activated in a mutual interplay.
There are six basic movement patterns which give quality information about the function of the motor system of the particular subject. These movements are: hip (hyper) extension, hip abduction, curl up from supine, head flexion, push up and shoulder abduction.
Treatment Proposal
The final goal of the therapeutic plan is to achieve the best possible movement patterns as a best possible prevention of recurrences of acute pain episodes.
The treatment proposal can be split into 3 basic steps:
Improvement of function of possibly all peripheral structures which show any kind of dysfunction, regardless whether painful or painless, as any dysfunction has to be considered as a source of impaired proprioceptive information. Based on the concept of motor learning, adequate information is essential to normalize the whole motor regulation.
Improvement of muscle imbalance as a presumption for improvement of the biomechanics. Treatment of tight muscles (stretching) should precede strengthening as tight muscles are not only readily activated but activated even during movements in which they should be silent. Therefore in presence of tight muscles it is impossible to strengthen specifically weakened muscles. This is one of the explanations why – if this rule is ignored – an exercise program fails.
Improvement of central nervous motor control, programming and improvement of motor units firing pattern in an attempt to speed up the muscle contraction and thus to improve the muscular protection of joints to prevent their injury. This in principle can be achieved in three ways, namely by
- Increasing of the proprioceptive flow from the periphery to facilitate the efferent motor system
- Activating systems which regulate co-ordination, posture and equilibrium (spino-cerebello-vestibular pathways)
- Using primitive reflex locomotion (reflex creeping and reflex crawling) and irritation of reflex zones to facilitate in particular deep intrinsic muscles of the spine and thus to improve the stabilization of the spine.